Care delivery re-imaged for the most complex, highest-cost patient populations
The eIAC ambulatory telehealth program is built upon a population management software platform designed for monitoring and delivering care to the most complex patients at home. Care systems develop the organizational capability to deliver integrated, coordinated care across specialties and services at scale. The eIAC program enables all stakeholders in the clinical and social management of a patient to identify and address the root causes of the patient’s frequent admissions, creating a cohesive system of care that helps reduce hospital admissions while providing the highest level of care to patients with complex, chronic conditions.¹
Intensive Ambulatory Care program: A holistic approach to patient care
Philips enterprise telehealth programs enable the transition to patient-centered, cost-effective, proactive health management and support pay-for-value care delivery.
Program features and services
By combining leading telehealth technologies that monitor and educate, with a transformed clinical model that unites former factionalized care team members, the eIAC program brings a concentration of effort to the small number of patients that utilize the majority of your system’s resources and funds.
Advanced algorithms
The eIAC program leverages Philips’ proprietary algorithms to select actionable patient populations for whom a coaching-focused ambulatory care model can make a significant impact. The eIAC program accounts for the dynamic nature of your patient populations and adapts to each patient‘s status to provide that you are proactively managing today’s highest-cost patients and making the most effective use of your resources.
Behavioral science foundation²
The platform and program are highly tailorable, so that care plans can be personalized to each patient's current behavior and readiness for change. Communications are tailored based on precise patient phenotyping. Behavioral science theory has been employed to shape eIAC program care experiences, providing the greatest chance of patient acceptance and adoption of proper self-care behaviors.
Clinical and operational support and training
The comprehensive eIAC program provides detailed designs and workflows that are underpinned by a technology platform that helps you rapidly stand up and scale your program. The Philips team is there at every step to provide you with the support and training required to start on the right path, grow you program and realize the clinical and financial outcomes you seek.
Platform for effective care collaboration
Complex patients require a multi-disciplinary team of clinicians and specialists. The eIAC program provides a platform for cross-functional care teams to collaborate in real-time on their highest-cost patients; and track and manage the physiological and psycho-social risk factors that might increase the chances of a hospital readmission.
Real-world results
Treating patients with complex chronic conditions—the most acute 5% of the patient population—often takes up 50% of a health system’s resources.³ The eIAC program can help lower the cost of quality care for these patients. In a study at Banner Health, the eIAC program¹:
Enabling technologies
-
eCareCoordinator
To learn more about Philips enterprise telehealth programs, please call us at 1-866-554-4776 or click below.
NOCTN482 -
eCareCompanion patient app
To learn more about Philips enterprise telehealth programs, please call us at 1-866-554-4776 or click below.
NOCTN483
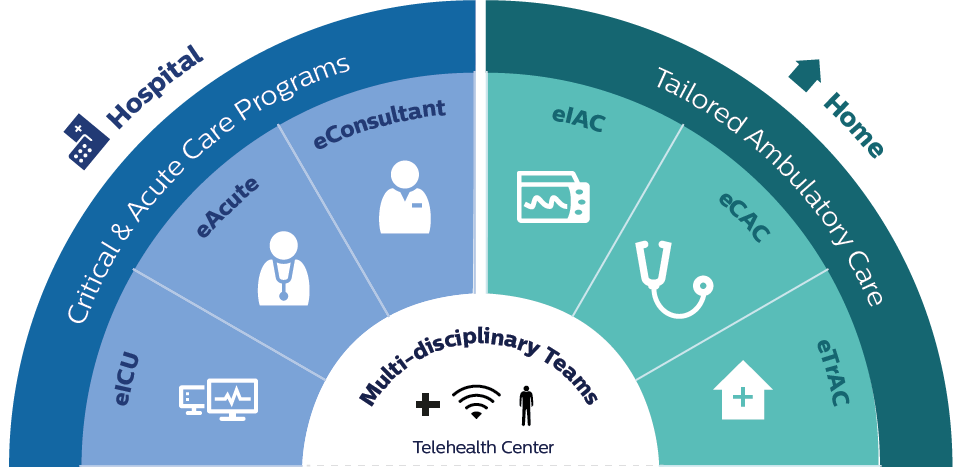
Connected, patient-centered care
Related offerings
Disclaimers